If it has been weeks or months since you hit your head, and you are still dealing with symptoms, it can start to feel confusing fast.
You might be told: "Your scans are clear." Or "Just rest." Or "It's anxiety." Or "It will pass."
And yet your body keeps sending the same message:
Something is still off.
This is the space where Post-Concussion Syndrome (PCS) lives. In this article, I will explain PCS in plain language, why symptoms can linger long after the original injury, and how Functional Neuro Health (FNH) approaches it differently — by working with the nervous system as the foundation of recovery.
What is Post-Concussion Syndrome?
A concussion is a type of traumatic brain injury. Many people recover fully with time, especially after a first concussion, and especially if they are well-managed early.
Post-Concussion Syndrome is when symptoms persist longer than expected. Symptoms lasting longer than about 3 weeks in adults (and 4 weeks in children) can fall into a post-concussion pattern.
That does not mean anything is "wrong with you" as a person. It means your nervous system is still in a protective mode, and it has not fully reorganised yet.
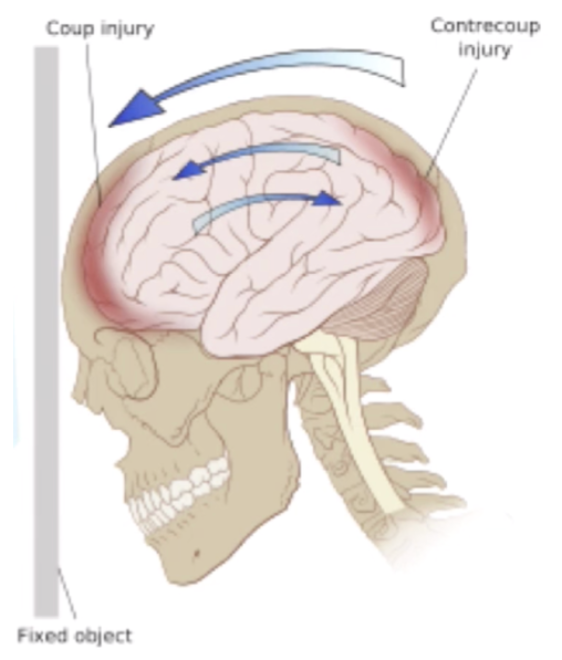
A concussion involves both the initial impact (coup) and a secondary contact as the brain moves inside the skull (contrecoup) — creating a cascade of effects throughout the nervous system.
Common Symptoms — and Why They Feel So Widespread
PCS symptoms can affect multiple areas at once, which is part of what makes it stressful. A lot of people get stuck here because it does not feel like one problem. But there is a unifying theme: your nervous system is dysregulated and disorganised.
Physical
- Headaches and pressure
- Neck pain
- Light or noise sensitivity
- Visual strain
- Dizziness and balance issues
- Nausea
Cognitive
- Brain fog
- Slower thinking
- Difficulty concentrating
- Memory issues
- Feeling 'not as sharp'
Emotional
- Anxiety and nervousness
- Irritability
- Low mood
- Feeling flat or 'not yourself'
- Feeling more reactive than usual
Sleep / Energy
- Fatigue
- Trouble falling asleep
- Sleeping more or less than normal
- Feeling wired-but-tired
Why Symptoms Can Persist: The Nervous System Is Still Protecting You
A concussion is not just a bump on the head. It is an event where the brain experiences sudden force — often including both the initial impact and a secondary contact inside the skull as the brain moves. That can create a cascade of effects:
1) A "Sensitised Brain" State
After concussion, the brain can become more reactive to inputs that used to be normal: busy environments, screen time, quick head movement, bright light, noise, stress, and exercise. This is why people sometimes say: "I feel like my senses are too loud."
2) An Energy Mismatch
After concussion, your brain may temporarily need more energy to function normally, while blood flow and metabolic efficiency can be reduced. So you get the classic PCS experience: "I can do things… but I crash faster than I should."
3) Neuroinflammation That Does Not Fully Settle
The brain has immune cells that help with repair and cleanup after injury. That is normal. But if the nervous system stays in threat, the inflammation response can stay "switched on" longer than it should. When that happens, you can feel like you are stuck in a loop: symptoms feed stress, stress feeds symptoms.
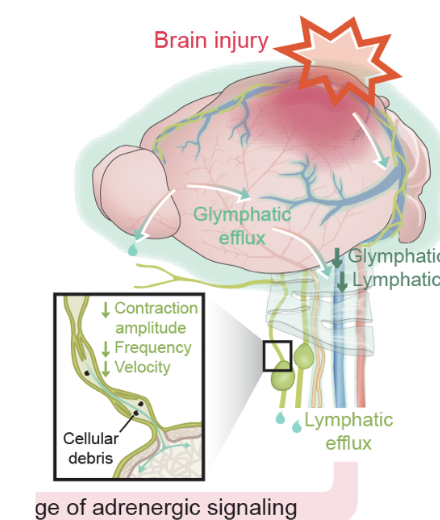
After brain injury, the glymphatic system — the brain's waste-clearance network — can become impaired, reducing the drainage of cellular debris and contributing to ongoing neuroinflammation.
4) The Gut–Brain Link (Yes, It Is Real)
After head trauma, the nervous system can shift how the gut functions, including motility and the integrity of the gut lining. That can contribute to gut symptoms that appear after concussion, increased sensitivity to foods, and an inflammatory load that keeps the system reactive.
This is one reason some "gut-only" approaches do not stick if the nervous system driver has not been addressed.
Why FNH Is Different: We Treat PCS as a System Problem, Not a Symptom Problem
Many approaches focus on symptom management — reduce headaches, reduce dizziness, reduce anxiety, improve sleep. Those can matter. But if the organising system (your nervous system) is still dysregulated, symptoms can keep returning.
At Functional Neuro Health, PCS is approached as a nervous system reorganisation process. We use the PEACE Method framework:
Preliminary Assessment
Map what is currently disorganised — balance, vision, breath, neck, and history.
Ease the System
Reduce threat load first. Breathing mechanics, lymphatic drainage, downshifting the stress response.
Align the Hierarchy
Identify what is primary today — sensory, nociceptive, autonomic, or gut/immune.
Correct
Targeted corrections at the minimum effective dose — cranial nerves, neck, eye systems, nociception.
Embed
One to three precise home drills, matched to your threshold, progressed safely over time.
What an In-Person PCS Session Looks Like at FNH
Step 1: Preliminary Assessment
We start with a careful history, because PCS is never "just the one hit." We look at where the impact happened, whether there were multiple concussions over time, neck involvement, whether there were other stresses or illnesses around the injury, and the symptom pattern: what flares it, what settles it.
We also do functional checks based on your presentation — often including balance and vestibular tolerance, eye coordination (tracking and convergence), breath and nervous system capacity, and neck function. We are not trying to provoke symptoms. We are mapping what is currently disorganised.


Balance and vestibular assessment is a key part of the PCS evaluation at FNH. Single-leg stance with eyes open and closed reveals how well the nervous system is integrating sensory information.
Step 2: Ease the System
PCS improves faster when the nervous system can come out of threat. So we often begin with high-leverage "ease" work — easing the breathing system (often via the phrenic nerve and diaphragm mechanics), supporting drainage and recovery, and downshifting the stress response so the brain can reorganise.
Many people expect "hard rehab" first. But with PCS, less is more early on. We want to get you under your threshold, not push you over it.
Step 3: Align the Hierarchy
PCS is layered. If you treat out of order, you can get stuck. So we ask: What is primary today? Is the system being driven most by sensory issues (vision/vestibular)? By neck and nociception? By autonomic dysregulation? By gut and immune layers? This step prevents random guessing.
Step 4: Correct
This is where targeted corrections happen — often around nociception (threat signalling from impact sites and neck), cranial nerves (especially those linked to vision, vestibular function, and vagal tone), eye systems (tracking, convergence, VOR), and neck stabilisers.
The goal is not to do everything. The goal is to deliver the minimum effective dose that creates a measurable shift.
Step 5: Embed
This is where you stop relying on the session and start building stability at home. PCS rehab is not about grinding harder. It is about the right drill, in the right position, at the right speed, for the right number of reps, without triggering symptoms.
You will typically leave with one to three priority home practices. And the rule is simple: we do not push you into symptoms. We train below your threshold so your brain can build capacity safely.
A Real Example: A "Two-Week Concussion" That Shifted Fast
A person was about two weeks post-injury, with symptoms like feeling foggy, flatter mood, some balance and coordination changes, and sleep not fully downshifting.
- 1.The session started by reducing load (breathing and diaphragm support, drainage).
- 2.The assessment mapped what was disorganised — balance and eye systems showed clear signals.
- 3.A key driver was addressed first: threat signalling from impact sites.
- 4.Many downstream issues improved once that primary driver was corrected.
- 5.The person left with very small, precise homework, matched to their tolerance.
Client takeaway: PCS recovery is often about sequencing. When you change the primary driver, the rest of the system has room to reorganise.
What You Can Do Now If You Suspect PCS
Take red flags seriously
If you have severe or worsening symptoms, seizures, repeated vomiting, major weakness or numbness, or anything that feels like an emergency — that is medical territory.
Stop trying to outwork your nervous system
PCS usually worsens when people repeatedly exceed their threshold.
Get assessed through a nervous system lens
The right assessment can reveal whether vision, vestibular, neck, breath capacity, or inflammation load is acting as the main driver.
Make rehab smaller, not bigger
If a drill makes you flare, it is not proof you are broken. It is proof the dose is wrong.
A Gentle Next Step
If you are weeks or months after a concussion and still feel "not right," it does not mean you are stuck forever.
It usually means your nervous system is still protecting you, and it needs the right sequence of inputs to reorganise.
The FNH approach is built for exactly that: restore safety first, correct what is primary, and embed change so it lasts.
Ready to take the next step?
Book a Neuro Health Assessment
A free 15-minute call to discuss your symptoms and whether the FNH approach is the right fit for you.
Book a Neuro Health AssessmentFrequently Asked Questions
What is the best treatment for post-concussion syndrome?
The most effective approach is active, targeted rehabilitation rather than prolonged rest. This includes vestibular therapy, vision rehabilitation, cervical physiotherapy, and nervous system regulation — matched to the specific drivers of your symptoms. A functional neurology assessment identifies which systems are most disrupted and sequences treatment accordingly.
How does a neurologist treat post-concussion syndrome?
A functional neurologist assesses the nervous system as a whole — evaluating eye movements, balance, vestibular function, cervical spine, breathing mechanics, and autonomic regulation. Treatment targets the specific neurological systems that are dysregulated, rather than managing individual symptoms in isolation.
How to reset your brain after a concussion?
Brain reset after concussion involves gradually re-exposing the nervous system to controlled stimulation — starting below your symptom threshold. This includes graded aerobic exercise, vestibular and vision rehabilitation, sleep optimisation, and nervous system downregulation techniques. The key principle: small, consistent inputs below the threshold that provokes symptoms, progressed carefully over time.
Why do post-concussion symptoms last so long?
Symptoms persist when the nervous system remains in a protective or dysregulated state after the initial injury has healed. The brain's threat-detection systems stay activated, maintaining fatigue, brain fog, light sensitivity, and anxiety even when structural damage is no longer present. This is why rest alone rarely resolves persistent PCS — the nervous system needs active rehabilitation.

Written by
Nick Moss
Applied Functional Neurologist · Founder of Functional Neuro Health · 10,000+ clinical hours · 15+ years experience
View full profile →Free Download
Why Your Body Isn't Broken
A practical guide to understanding why chronic symptoms persist — and what a nervous system-first approach can do when conventional treatment has failed. Free to download.

